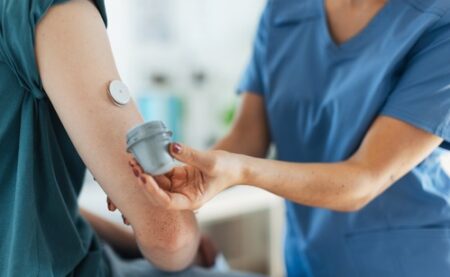
Pediatric Endocrinology Nurse Career Overview
What Is a Pediatric Endocrinology Nurse?
Pediatric endocrinology nurses care for children and infants with endocrine disorders. The endocrine system is made up of glands throughout the body and the various hormones they release. Growth hormone holds special significance for children, as any interruption in its release can impede growth and development.
In another example, glands in the pancreas secrete a hormone called insulin, which regulates blood sugar. When this process malfunctions, patients develop diabetes. Type 1 diabetes is the most common endocrine disorder in children, and pediatric endocrinology nurses become very familiar with its symptoms and treatment.
How Long to Become?
2-4 Years
Job Outlook
6% increase from 2022 to 2032
Average Salary
$94,480
Where Do Pediatric Endocrinology Nurses Work?
Pediatric patients with endocrinology disorders may seek care as outpatients, but occasionally, they must be admitted to the hospital. As a result, pediatric endocrinology nurses can find work in a variety of areas:
- Hospitals
- Pediatrician offices
- Outpatient clinics
- Community centers
- Home health companies
In the hospital, pediatric endocrinology nurses care for patients during an acute illness flare-up. In diabetes, for example, if a child’s blood sugar gets too high or too low, they must receive rapid care to correct those levels. An endocrinology nursing role in the hospital requires quick thinking and attention to detail. In offices and outpatient settings, pediatric endocrinology nurses help patients prevent acute illness through care and education.
No matter where pediatric endocrinology nurses work, they may see these common endocrine diagnoses:
- Adrenal insufficiency/Addison’s disease
- Delayed puberty
- Diabetes insipidus
- Diabetes mellitus
- Disorders of sexual development
- Growth hormone deficiency
- Hyperthyroidism/hypothyroidism
- Klinefelter syndrome
- Overactive adrenal glands/Cushing’s syndrome
- Polycystic ovary syndrome
- Precocious puberty
- Turner syndrome
What Does a Pediatric Endocrinology Nurse Do?
Pediatric endocrinology nurses may find their daily tasks differ between hospital and outpatient care. In a provider office or clinic, pediatric endocrinology nurses may check point-of-care labs like blood glucose testing, educate patients and families, and answer patient’s questions when they call. In the hospital, pediatric endocrinology nurses may have some additional tasks, like:
- Central line management (like ports and PICCs)
- Collaboration with other health team members
- Collection of blood and other bodily fluids for laboratory testing
- Coordination of care with other departments
- Educate patients and families on insulin calculation
- Emergency resuscitation
- Frequent blood glucose level monitoring
- Head-to-toe assessment
- Insertion and management of foley catheters
- IV insertion and maintenance
- Medication administration
- Patient hygiene and comfort
- Patient transportation
- Vital signs monitoring
No matter the setting, pediatric endocrinology nurses must be able to establish a rapport with young patients, helping them feel comfortable and safe. An endocrinology illness is often permanent, and nurses in this specialty can help patients learn how to manage it well and live a long, full life.
How Do I Become a Pediatric Endocrinology Nurse?
Aspiring pediatric endocrinology nurses have to start by earning a nursing degree from an accredited nursing program. Pediatric endocrinology nurses can choose to pursue an Associate Degree in Nursing (ADN) or a Bachelor of Science in Nursing (BSN). However, more and more facilities require a BSN for pediatric endocrinology care.
After graduation, new nurses can apply to work in a pediatric endocrinology setting as graduate nurses (GNs). They can practice as GNs under a nurse preceptor – an experienced nurse who trains new nurses. After they pass the National Council Licensure Examination (NCLEX-RN), their state licensing exam, GNs become registered nurses (RNs). After they finish training in their unit or office, pediatric endocrinology nurses can practice on their own.
In almost all health settings, pediatric endocrinology nurses will be required to obtain their Basic Life Support (BLS) certification. On some hospital units, a Pediatric Advanced Life Support (PALS) certification is highly encouraged.
Once a pediatric endocrinology nurse has some experience in the field, they may want to earn a specialty certification. While there is no specific certification for endocrinology nursing, nurses can choose from specialty designations like:
Most specialty certifications require nurses to have a valid license and a certain number of years or hours of experience in that specialty before they can take the certification exam.
Beyond certification, pediatric endocrinology nurses can also return to school for an advanced practice degree. After graduating with a Master of Science in Nursing (MSN) with a focus on pediatric endocrinology, nurses can practice as nurse practitioners (NPs). It’s possible to graduate with an MSN within two years, but many nurses choose to take longer so they can continue working full-time during the program.
Another advanced-degree path nurses may take is to become a clinical nurse specialist. These nurses have an MSN and specialize in one area of nursing, like endocrinology. While both NPs and clinical nurse specialists perform patient care by assessing patients and prescribing treatment, clinical nurse specialists lean toward improving patient care as a whole. They can also serve as nurse educators and be a resource for RNs on their team.
Endocrine diseases are complex, and a large part of an endocrinology nurse’s job is to educate patients and families on their medical issues. Diabetic management, for example, requires patients or parents to closely monitor what the patient eats, calculate the carbohydrates in each meal or snack, and then apply a mathematical formula to decide how much insulin to give. Once patients get used to this process, they can do it in their sleep, but first, they need copious support from their nurses.
How Much Does a Pediatric Endocrinology Nurse Make Per Year?
Pediatric endocrinology nurses’ salaries are similar to that of other RNs and can vary greatly by employer, location, and experience. The average annual pay for RNs is $94,480 a year, according to the Bureau of Labor Statistics (BLS). The median pay represents the middle: half of RNs earned more than that amount, and half earned less.
Depending on where you work, your employer may be able to offer higher or lower compensation:
- General Medical and Surgical Hospitals: $96,830
- Outpatient Care Centers: $102,640
- Offices of Physicians: $83,110
- Home Health Care Services: $87,430
Salaries also vary depending on which state a pediatric endocrinolgy nurse practices. The West Coast generally pays nurses the best, but they also have a higher cost of living.
Annual Mean Wage of Registered Nurses, by State
- $69,030 - $80,760
- $81,390 - $86,210
- $87,220 - $94,670
- $94,830 - $137,690
Blank areas indicate data not available
The top-paying areas for pediatric endocrinology nurses include:
- San Francisco-Oakland-Hayward, CA: $174,370
- Vallejo-Fairfield, CA: $171,620
- San Jose-Sunnyvale-Santa Clara, CA: $170,780
- Napa, CA: $166,180
- Sacramento–Roseville–Arden-Arcade, CA: $154,510
- Santa Rosa, CA: $152,930
- Modesto, CA: $145,190
- Santa Cruz-Watsonville, CA: $140,880
- San Luis Obispo–Paso Robles–Arroyo Grande, CA: $140,560
- Stockton-Lodi, CA: $138,420
Are Pediatric Endocrinology Nurses in High Demand?
According to the Centers for Disease Control, 283,000 children and adolescents under 20 (35 per 10,000 US youths) were diagnosed with diabetes in 2019, and 244,000 of those had type 1 diabetes. In 2020, diabetes diagnoses in children went up, and providers who specialize in endocrinology are in short supply. “The pediatric endocrinology workforce, once projected to be in surplus, is now struggling to sustain an adequate, let alone optimal capacity,” reads a report by the Association Of Medical School Pediatric Department Chairs.
And it’s not just endocrinology – all nursing specialties are currently in high demand in the United States. According to the U.S. Department of Health and Human Services, 24% of U.S. hospitals have reported critical staffing shortages. As long as the nursing shortage continues, pediatric endocrinology nurses will remain in high demand.
Additional Resources for Pediatric Endocrinology Nurses
To learn more about becoming a pediatric endocrinology nurse, these additional resources may help: